How We’re Helping COVID-19 Patients Breathe and Communicate
When patients arrive at The New Jewish Home with tracheostomies after being hospitalized for COVID-19, their speech, breathing and swallowing are impaired. Our Department of Speech-Language and Swallowing Disorders — known for its excellent care — is dedicated to improving the quality of life for patients like these.
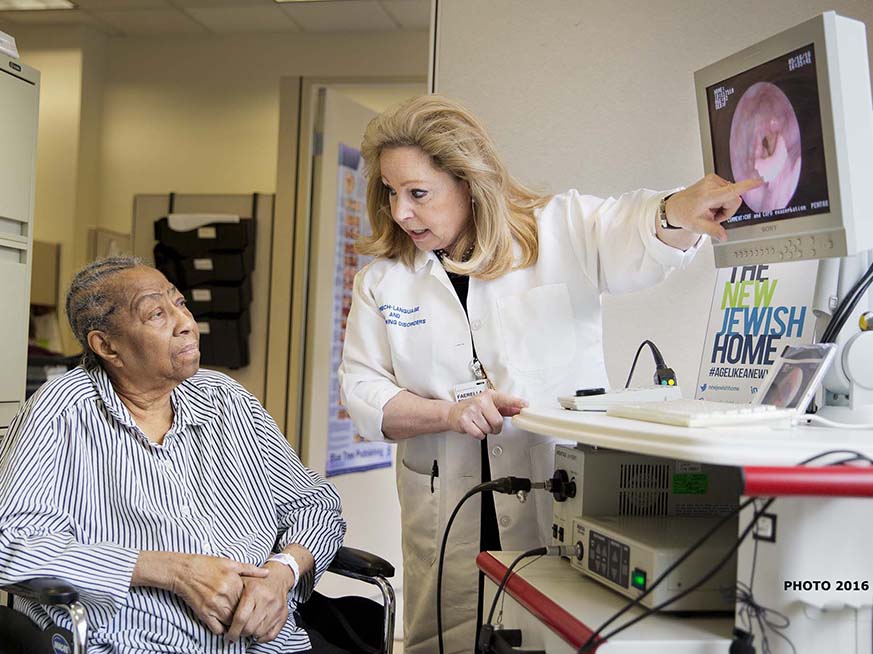
Faerella (Fae) Boczko is the chief of the department and a Board-Certified Specialist in Swallowing and Swallowing Disorders with more than 32 years of experience in geriatric care. We asked her what makes this department so successful and unique, and how the coronavirus pandemic is impacting her work.
Tell us about the work that gets done in the Department of Speech-Language and Swallowing Disorders.
Our highly skilled speech pathologists see about 30 patients a day — five days a week — all year long. We treat patients with speech, language, cognitive impairment and swallowing disorders. This can include brain injury, stroke, cancer, multiple sclerosis, Parkinson’s and other neuromuscular and neurological conditions — and these days, many COVID-19 patients. All of the patients we see are transferred to us from hospitals. Here at The New Jewish Home, they receive life-changing post-hospitalization care.
How has your work been affected by COVID-19?
Recently, as a result of the pandemic, we have received a lot of post-acute patients coming in from the hospital with tracheostomies of different types and different sizes. They are so debilitated — some of these patients are so weak they can’t even use a call bell.
We work with the patients on coordinating swallowing and breathing. It is difficult for them to communicate, so sometimes we use a communication board or a book where they can indicate letters, words, or images. Or they may need to gesture or write out their messages. When they are able to tolerate a speaking valve, we’ll introduce that, to begin verbal communication. We have been very successful in weaning patients from the trach, working with them step by step to a point where they no longer need it. They are overwhelmed with joy.
Tell us about some of the COVID patients you have worked with.
I met a woman – let’s call her Mrs. T – who came to The New Jewish Home after being in the hospital for more than a month. She had respiratory failure and had been intubated, and she arrived here with a rather large trach and a feeding tube. Mrs. T was unable to speak and unable to swallow, using hand gestures to communicate. Before her illness she was a relatively healthy woman, and now she was quite weak and felt very down.
First I worked with Mrs. T to see if she could maintain breathing by covering the trach opening, then I introduced the speaking valve to see how long she could tolerate it, starting with just five minutes, and working up to ten minutes, an hour, two hours. Patients begin to feel better when they can use their voice. Her trach is now out and she’s sitting up in a wheelchair. Although the patient still has a feeding tube, Mrs. T. has moved to pureed meals, which has made her very happy.
A gentleman we’re working with experienced respiratory failure and had a large trach. He could not speak, so he shook his head to signal “yes” and “no” and tried to write a little. When he was finally able to tolerate the speaking valve, his response was, “Having a voice back makes me feel so connected. Thank goodness I can actually begin to talk.”
How important is it to get the family or caregivers involved in your therapy?
It’s critically important! We involve the families as much as possible. We call them immediately to explain our findings and our plan. We explain the physiology and the mechanics of swallowing.
Normally, we invite families to come in so they can attend therapy sessions. These days, when families aren’t able to come in to visit due to COVID-19, it’s more critical than ever to help patients get to the point where they can call a family member, with assistance.
We invite — and even urge — family members and caregivers to work with us. Letting them see the personalized studies we’ve done for their family member helps them better understand what’s going on physiologically so they can contribute to the person’s recovery.
In one very emotional case, we worked with a patient who was on a continuous feeding tube. He was constantly drooling and had to wipe with a towel all day long. He was embarrassed in front of his daughter. He told me he felt like he was hostage to the feeding tube.
So when we began intensive therapy with him, we slowly brought his daughter in to understand what was happening with her father. We helped her understand her father’s ability and she learned what he needed to do to be able to swallow. This eased his embarrassment and helped their relationship.
There are other skilled nursing facilities that offer similar services, but what sets your department apart from all the others?
First, I’m proud to say that we are the only skilled nursing facility in Manhattan with a full-time, board-certified specialist in speech-language and swallowing disorders. Every person who comes to The New Jewish Home in Manhattan is screened for speech, language and swallowing disorders. The department is current and up to date on the latest scientific research and uses evidence-based treatments. We complete standardized diagnostic batteries that other facilities may not use. We use electromyographic bio feedback and the Iowa Oral Performance Instrument (IOPI) which helps build tongue strength and endurance. We perform fiber-optic endoscopic evaluations of swallowing.
With patients who are accustomed to working with computers, we find technology, like tablets, particularly effective. Using certain programs, we challenge patients to complete language and speech tasks. This technology is very motivating and successfully engages the patients who really benefit from the immediate feedback.
We had one patient who could not express herself and was having difficulty communicating with her family. She used programs on the tablet and re-learned to use the telephone and is now able to call her sister. This small accomplishment had a major impact on improving her quality of life.
How do you help patients believe that they can overcome their serious disabilities or medical problems?
In some cases, before they come to us, the patients are told, “You’ll never swallow again. You’ll never speak again.”
But then, they come to us and we see the possibilities. We never look at what our patients cannot do, but rather, what they can do. And we build on that. That’s what makes us different. It’s all about compassion and kindness and restoring confidence and dignity to patients who have often lost all hope.
In addition to the extraordinary medical care you and your team provide, how much of what you do is about restoring human dignity to your patients’ lives?
That’s what it’s all about! You take someone who had been in a hospital, someone who’s depressed, someone who’s come to us broken with barely a glimmer of hope. They are weak and deconditioned and they come to us believing they can never go back to eating or speaking.
And we show them the possibilities! We treated a patient who had his tongue removed — the result of cancer. When he came to us, he couldn’t eat. We taught him how to hold food in his mouth and how to swallow. Watching the joy on his face when he was able to eat mashed potatoes for the first time — you can’t put those feelings into words.
You’ve been doing this work for more than three decades, Fae. Why do you still do it?
The immense satisfaction I get when I see patients benefitting from our hard work is beyond compare. In this department, we are changing lives for the better every day. The gratitude we get from our patients and their families makes the long hours and the hard work all worth it.
The New Jewish Home has a proud legacy of empowering older adults to live with purpose and enhanced well-being. We’ve been around since 1848 as one of the nation’s first nursing homes, and now serving older New Yorkers of all backgrounds through a portfolio of health care services, including post-acute care and rehabilitation, skilled nursing, adult day care, assisted living, and at-home care.
See how we continue to elevate health care for older adults through our Research Institute on Aging and our SkillSpring program (formerly known as Geriatrics Career Development program), which empower teens and young adults to begin careers in health care.